Quick Overview
“Genital Herpes” refers to a sexually-transmitted virus (HSV-2)
Genital herpes (HSV-2) can’t be cured but the severity of symptoms and the length of time you have outbreak can be minimized by taking a prescription medication
The anti-viral, prescription medications used to treat cold sores (HSV-1) need to be taken as fast as possible
What is Herpes Simplex Virus Type 2?
If you find red sores that are sensitive to touch on or near your genitals or around your anal area, you may be experiencing the beginning of a herpes simplex virus type 2 (HSV-2) outbreak.
There are two classifications of herpes infections, and you can generally tell which one you have by the area on your body where the symptoms surface.
Herpes simplex virus type 2
(HSV-2)
also known as genital herpes, is usually spread through sexual intercourse, oral sex, or other skin-to-skin contact. The infection can cause sores on the penis, vagina, anus, or buttocks, and is sometimes found in other locations below the waist.
Neither HSV-1 nor HSV-2 are curable, but they can be treated with medication to eliminate the extent and duration of an outbreak. It is possible to go for months or years without symptoms; however, the virus never leaves the nerve cells so an outbreak can potentially occur at any time.
In this post, we will focus on the symptoms and treatment of HSV-2.
To help you determine whether you may be in the midst of an HSV-2 outbreak, we’ve put together an easy-to-understand overview of telltale symptoms so you can decide whether you need to pursue treatment.
While many people are naturally frustrated with genital herpes, the good news is that if you address a herpes outbreak early and secure a prescription from a doctor immediately, you can substantially minimize the symptoms and limit the risk of infecting others.
ABOUT HSV-2
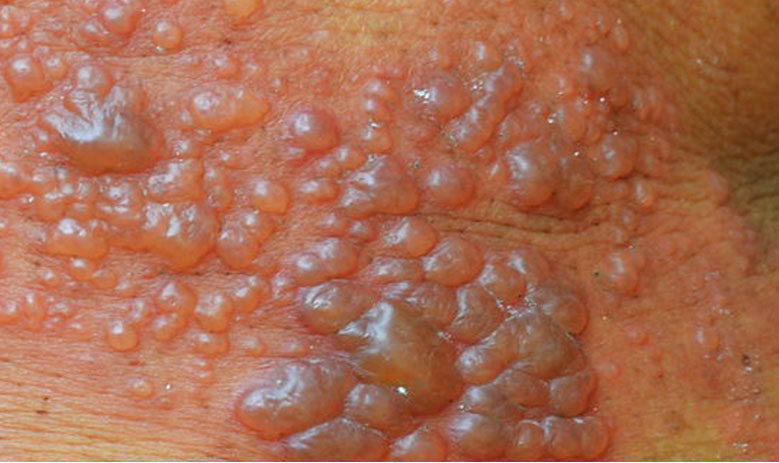
Many people infected with HSV-2 have no symptoms or mistakenly assume they have a different skin condition like a pimple or ingrown hairs; Sometimes people even think they experienced a “spider bite” or that they are experiencing “chafing” from exercising. That’s why it’s critical to understand what distinguishes herpes from other infections. Otherwise, because it’s so contagious, you may unintendedly spread it to your sexual partner without realizing it.
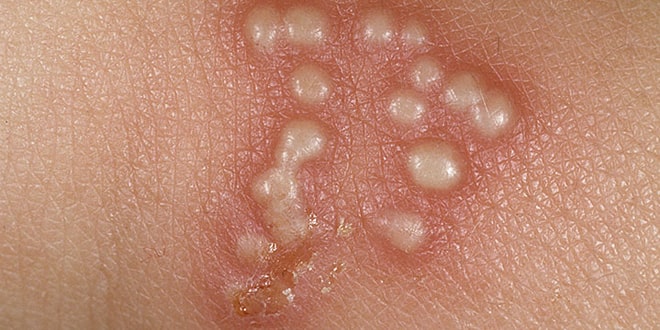
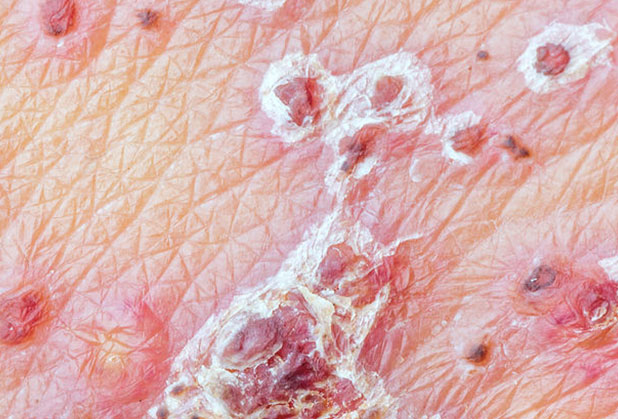
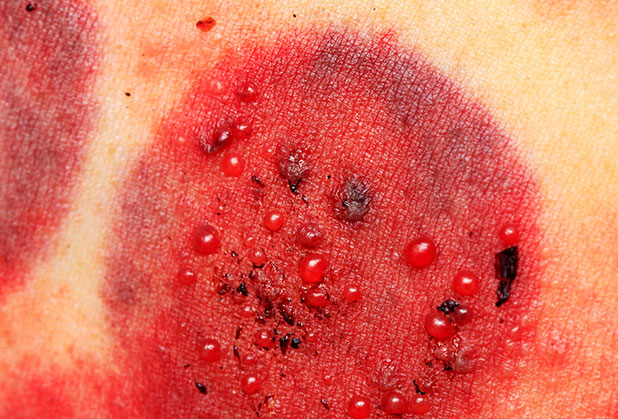
The visible signs of genital herpes begin with an initial reddening of the skin, followed by irritation or itchiness, much like a rash. Soon after, blisters filled with clear fluid begin to form. Herpes blisters are often tender, and can be uncomfortable or even painful. Mild to severe itching can occur. Eventually the blisters pop and discharge, resulting in open sores or ulcers which later crust over signaling the beginning of a long healing process.
Herpes blisters are typically 1 to 3 millimeters in size and may appear alone or in crops made up of multiple sores. On men, they are usually found on or around the penis. On women, they may appear on the outside or inside of the vagina. They can also be found in and around the anal area.
Other signs of an outbreak may include:
- Flu-like symptoms, such as a fever, headache, muscle aches or swollen lymph node glands
- A burning sensation or discomfort while urinating
- Vaginal or penile discharge
- Itching in the ano-genital region
- Generalized irritability
An HSV-2 episode can take up to four weeks to clear up, but when addressed at an early stage in the outbreak lifecycle, prescription medication can help speed up the healing process.
There are some early signs that can indicate an outbreak is coming, but these are often overlooked by people who don’t know they have herpes. Most commonly reported by patients who recognize the warning signals is an itchy, tingling sensation on the skin, anywhere from a few hours to a couple of days prior to seeing herpes develop on the skin.
People contract genital herpes through direct contact with an infected sexual partner. Any type of skin-on-skin contact can spread herpes, but most often it’s done through sexual intercourse and oral sex. That’s because herpes gets access to the body through broken skin or a mucous membrane.
While some herpes cases are the result of a knowingly infected person who neglected to be honest with their partner, herpes can also be spread when there are no symptoms present by a partner who is not even aware they have it.
Although it doesn’t happen that often, someone infected with HSV-1 can transmit HSV-2 to a partner through oral-to-genital contact.
Because HSV-2 is highly contagious, it’s important for anyone with potential symptoms to be diagnosed and get treatment as soon as possible, in order to prevent spreading it to more people.

Genital herpes symptoms can begin to develop anywhere from 2 to 14 days after you’ve had exposure to someone with genital herpes. Other subtle symptoms besides sores or lesions may be present, but they usually aren’t recognizable by people experiencing their first herpes outbreak.
If you think you may have genital herpes, it is always advisable to avoid sexual contact from the first sign of symptoms until two to three days after the outbreak has cleared. Even with a condom, herpes can still be passed from one person to another.
The risk of contracting genital herpes is highest during an outbreak, but it is possible to transmit the virus when symptoms aren’t present. This is due to asymptomatic viral shedding, which is when the herpes virus is invisibly active and sheds at the site of infection. Viral shedding can last for 3 days, but because it cannot be seen by the naked eye, people often don’t realize they’ve been infected.
The good news is, if you catch the beginning of a herpes outbreak and seek immediate treatment, you can prevent the duration and severity of the symptoms.
Although there are no hard and fast rules for when someone with HSV-2 will present symptoms, there are some occasions where people are more susceptible to an outbreak.
They are:
- Physical stress or fatigue
- Emotional stress like depression or anxiety
- Sickness or infection where the immune system is compromised
- Fever or flu or illness
- Trauma (emotional or physical)
- Surgery
- Prolonged sun exposure (the sun suppresses your immune system leaving the HSV-2 virus unchecked)
- Hormone fluctuations (usually more common in women)
- Menstruation
- Pregnancy
- Friction caused by excessive sex or masturbation
- No real discernable reason at all

To determine whether you have HSV-2, it is best to have a doctor experienced with STDs look at your symptoms. Most doctors can easily differentiate herpes from other skin conditions with a visual exam. If they’re not sure, they may take a culture or extract a sample of fluid from the blisters, or in rare cases they can take a blood test to see if there are herpes antibodies present.

If you seek treatment for herpes the moment you notice symptoms, medication can help shorten the length of a herpes outbreak.
You can wait out a herpes outbreak and the sores will eventually heal, but it can take upwards of three to four weeks until that happens. People who are casually dating or in new relationships usually choose treatment so they can continue their day-to-day lives with minimal disruption.
A doctor can prescribe one of several medications to help ease genital herpes symptoms, thereby dramatically decreasing the length of an outbreak. But treatment must be sought quickly because the window of time when a herpes outbreak can be mitigated by medicine is limited.
Common medications prescribed for herpes HSV-2 are Acyclovir, Famciclovir, and Valacyclovir. Regardless of the medication, to be effective the first dosage should be taken within 12 to 24 hours of when the outbreak started.
There are also antiviral prescription creams that can lessen the discomfort caused by herpes sores or lesions.
There are over-the-counter medications that claim to help herpes, but there is no evidence to support that claim. The medications that have been proven to help treat herpes symptoms and decrease the length of an outbreak are available only with a prescription from a doctor.

Although not always active, the herpes infection never leaves the body. It is possible to have multiple outbreaks over the course of a year or a lifetime. How often someone experiences outbreaks depends largely on the individual and their health. Fortunately, repeat outbreaks are almost always less severe than the initial outbreak.
For the most part, genital herpes does not pose any major threats besides the stigma that’s attached to it.
However, during pregnancy HSV-2 can lead to issues in the developing fetus or newborn baby. Although it can be passed to an unborn child before birth, it is usually passed during delivery. In babies, herpes, referred to as neonatal herpes, can be fatal. Therefore, if you are pregnant, it is highly advisable that you seek immediate medical attention during a herpes outbreak. .
